Urethral Cancer Treatment (PDQ®): Treatment - Patient Information [NCI]
This information is produced and provided by the National Cancer Institute (NCI). The information in this topic may have changed since it was written. For the most current information, contact the National Cancer Institute via the Internet web site at http://cancer.gov or call 1-800-4-CANCER.
General Information About Urethral Cancer
Urethral cancer is a disease in which malignant (cancer) cells form in the tissues of the urethra.
The urethra is the tube that carries urine from the bladder to outside the body. In women, the urethra is about 1½ inches long and is just above the vagina. In men, the urethra is about 8 inches long, and goes through the prostate gland and the penis to the outside of the body. In men, the urethra also carries semen.
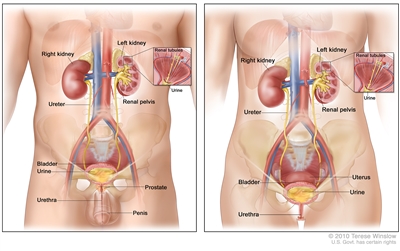
Anatomy of the male urinary system (left panel) and female urinary system (right panel) showing the kidneys, ureters, bladder, and urethra. The inside of the left kidney shows the renal pelvis. An inset shows the renal tubules and urine. Also shown are the prostate and penis (left panel) and the uterus (right panel). Urine is made in the renal tubules and collects in the renal pelvis of each kidney. The urine flows from the kidneys through the ureters to the bladder. The urine is stored in the bladder until it leaves the body through the urethra.
Urethral cancer is a rare cancer that occurs more often in men than in women.
There are different types of urethral cancer that begin in cells that line the urethra.
These cancers are named for the types of cells that become malignant (cancer):
- Squamous cell carcinoma is the most common type of urethral cancer. It forms in the thin, flat cells in the part of the urethra near the bladder in women, and in the lining of the urethra in the penis in men.
- Transitional cell carcinoma forms in the area near the urethral opening in women, and in the part of the urethra that goes through the prostate gland in men.
- Adenocarcinoma forms in the glands that are around the urethra in both men and women.
Urethral cancer can metastasize (spread) quickly to tissues around the urethra and is often found in nearby lymph nodes by the time it is diagnosed.
A history of bladder cancer can affect the risk of urethral cancer.
Anything that increases your chance of getting a disease is called a risk factor. Having a risk factor does not mean that you will get cancer; not having risk factors doesn't mean that you will not get cancer. Talk with your doctor if you think you may be at risk. Risk factors for urethral cancer include the following:
- Having a history of bladder cancer.
- Having conditions that cause chronic inflammation in the urethra, including:
- Sexually transmitted diseases (STDs), including human papillomavirus (HPV), especially HPV type 16.
- Frequent urinary tract infections (UTIs).
Signs of urethral cancer include bleeding or trouble with urination.
These and other signs and symptoms may be caused by urethral cancer or by other conditions. There may be no signs or symptoms in the early stages. Check with your doctor if you have any of the following:
- Trouble starting the flow of urine.
- Weak or interrupted ("stop-and-go") flow of urine.
- Frequent urination, especially at night.
- Incontinence.
- Discharge from the urethra.
- Bleeding from the urethra or blood in the urine.
- A lump or thickness in the perineum or penis.
- A painless lump or swelling in the groin.
Tests that examine the urethra and bladder are used to diagnose urethral cancer.
The following tests and procedures may be used:
- Physical exam and health history: An exam of the body to check general signs of health, including checking for signs of disease, such as lumps or anything else that seems unusual. A history of the patient's health habits and past illnesses and treatments will also be taken.
- Pelvic exam: An exam of the vagina, cervix, uterus, fallopian tubes, ovaries, and rectum. A speculum is inserted into the vagina and the doctor or nurse looks at the vagina and cervix for signs of disease. The doctor or nurse also inserts one or two lubricated, gloved fingers of one hand into the vagina and places the other hand over the lower abdomen to feel the size, shape, and position of the uterus and ovaries. The doctor or nurse also inserts a lubricated, gloved finger into the rectum to feel for lumps or abnormal areas.
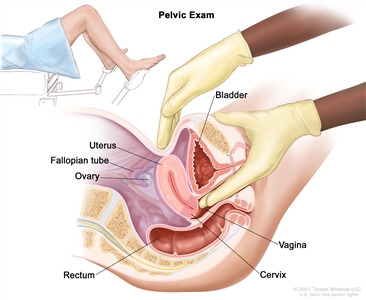
Pelvic exam. A doctor or nurse inserts one or two lubricated, gloved fingers of one hand into the vagina and presses on the lower abdomen with the other hand. This is done to feel the size, shape, and position of the uterus and ovaries. The vagina, cervix, fallopian tubes, and rectum are also checked. - Digital rectal exam: An exam of the rectum. The doctor or nurse inserts a lubricated, gloved finger into the lower part of the rectum to feel for lumps or anything else that seems unusual.
- Urine cytology: A laboratory test in which a sample of urine is checked under a microscope for abnormal cells.
- Urinalysis: A test to check the color of urine and its contents, such as sugar, protein, blood, and white blood cells. If white blood cells (a sign of infection) are found, a urine culture is usually done to find out what type of infection it is.
- Blood chemistry studies: A procedure in which a blood sample is checked to measure the amounts of certain substances released into the blood by organs and tissues in the body. An unusual (higher or lower than normal) amount of a substance can be a sign of disease.
- Complete blood count (CBC): A procedure in which a sample of blood is drawn and checked for the following:
- The number of red blood cells, white blood cells, and platelets.
- The amount of hemoglobin (the protein that carries oxygen) in the red blood cells.
- The portion of the blood sample made up of red blood cells.
- CT scan (CAT scan): A procedure that makes a series of detailed pictures of areas inside the body, such as the pelvis and abdomen, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography.
- Ureteroscopy: A procedure to look inside the ureter and renal pelvis to check for abnormal areas. A ureteroscope is a thin, tube-like instrument with a light and a lens for viewing. The ureteroscope is inserted through the urethra into the bladder, ureter, and renal pelvis. A tool may be inserted through the ureteroscope to take tissue samples to be checked under a microscope for signs of disease.
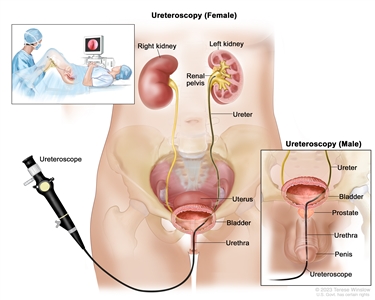
A ureteroscopy is a procedure that uses a ureteroscope (a thin, tube-like instrument with a light and a lens for viewing) to look inside the ureter and renal pelvis to check for abnormal areas. The ureteroscope is inserted through the urethra into the bladder, ureter, and renal pelvis. - Biopsy: The removal of cell or tissue samples from the urethra, bladder, and, sometimes, the prostate gland. The samples are viewed under a microscope by a pathologist to check for signs of cancer.
Certain factors affect prognosis (chance of recovery) and treatment options.
The prognosis and treatment options depend on the following:
- Where the cancer formed in the urethra.
- Whether the cancer has spread through the mucosa lining the urethra to nearby tissue, to lymph nodes, or to other parts of the body.
- Whether the patient is a male or female.
- The patient's general health.
- Whether the cancer has just been diagnosed or has recurred (come back).
Stages of Urethral Cancer
After urethral cancer has been diagnosed, tests are done to find out if cancer cells have spread within the urethra or to other parts of the body.
The process used to find out if cancer has spread within the urethra or to other parts of the body is called staging. The information gathered from the staging process determines the stage of the disease. It is important to know the stage in order to plan treatment.
The following procedures may be used in the staging process:
- Chest x-ray: An x-ray of the organs and bones inside the chest. An x-ray is a type of energy beam that can go through the body and onto film, making a picture of areas inside the body.
- CT scan (CAT scan) of the pelvis and abdomen: A procedure that makes a series of detailed pictures of the pelvis and abdomen, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography.
- MRI (magnetic resonance imaging): A procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of the urethra, nearby lymph nodes, and other soft tissue and bones in the pelvis. A substance called gadolinium is injected into the patient through a vein. The gadolinium collects around the cancer cells so they show up brighter in the picture. This procedure is also called nuclear magnetic resonance imaging (NMRI).
- Urethrography: A series of x-rays of the urethra. An x-ray is a type of energy beam that can go through the body and onto film, making a picture of areas inside the body. A dye is injected through the urethra into the bladder. The dye coats the bladder and urethra and x-rays are taken to see if the urethra is blocked and if cancer has spread to nearby tissue.
There are three ways that cancer spreads in the body.
Cancer can spread through tissue, the lymph system, and the blood:
- Tissue. The cancer spreads from where it began by growing into nearby areas.
- Lymph system. The cancer spreads from where it began by getting into the lymph system. The cancer travels through the lymph vessels to other parts of the body.
- Blood. The cancer spreads from where it began by getting into the blood. The cancer travels through the blood vessels to other parts of the body.
Cancer may spread from where it began to other parts of the body.
When cancer spreads to another part of the body, it is called metastasis. Cancer cells break away from where they began (the primary tumor) and travel through the lymph system or blood.
- Lymph system. The cancer gets into the lymph system, travels through the lymph vessels, and forms a tumor (metastatic tumor) in another part of the body.
- Blood. The cancer gets into the blood, travels through the blood vessels, and forms a tumor (metastatic tumor) in another part of the body.
The metastatic tumor is the same type of cancer as the primary tumor. For example, if urethral cancer spreads to the lung, the cancer cells in the lung are actually urethral cancer cells. The disease is metastatic urethral cancer, not lung cancer.
Urethral cancer is staged and treated based on the part of the urethra that is affected.
Urethral cancer is staged and treated based on the part of the urethra that is affected and how deeply the tumor has spread into tissue around the urethra. Urethral cancer can be described as distal or proximal.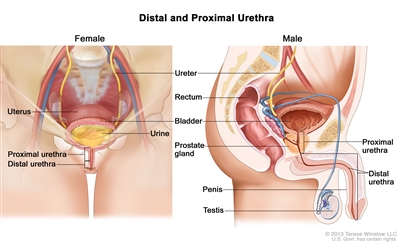
Anatomy of the distal and proximal urethra. Urine flows out of the bladder and leaves the body through the urethra. The part of the urethra that is closest to the bladder is called the proximal urethra. The part that is closest to where the urine leaves the body is called the distal urethra. The urethra is about 8 inches long in men and about 1½ inches long in women.
Distal urethral cancer
In distal urethral cancer, the cancer usually has not spread deeply into the tissue. In women, the part of the urethra that is closest to the outside of the body (about ½ inch) is affected. In men, the part of the urethra that is in the penis is affected.
Proximal urethral cancer
Proximal urethral cancer affects the part of the urethra that is not the distal urethra. In women and men, proximal urethral cancer usually has spread deeply into tissue.
Bladder and/or prostate cancer may occur at the same time as urethral cancer.
In men, cancer that forms in the proximal urethra (the part of the urethra that passes through the prostate to the bladder) may occur at the same time as cancer of the bladder and/or prostate. Sometimes this occurs at diagnosis and sometimes it occurs later.
Urethral cancer can recur (come back) after it has been treated.
The cancer may come back in the urethra or in other parts of the body.
Treatment Option Overview
There are different types of treatment for patients with urethral cancer.
Different types of treatments are available for patients with urethral cancer. Some treatments are standard (the currently used treatment), and some are being tested in clinical trials. A treatment clinical trial is a research study meant to help improve current treatments or obtain information on new treatments for patients with cancer. When clinical trials show that a new treatment is better than the standard treatment, the new treatment may become the standard treatment. Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
The following types of treatment are used:
Surgery
Surgery to remove the cancer is the most common treatment for cancer of the urethra. One of the following types of surgery may be done:
- Open excision: Removal of the cancer by surgery.
- Transurethral resection (TUR): Surgery to remove the cancer using a special tool inserted into the urethra.
- Electroresection with fulguration: Surgery to remove the cancer by electric current. A lighted tool with a small wire loop on the end is used to remove the cancer or to burn the tumor away with high-energy electricity.
- Laser surgery: A surgical procedure that uses a laser beam (a narrow beam of intense light) as a knife to make bloodless cuts in tissue or to remove or destroy tissue.
- Lymph node dissection: Lymph nodes in the pelvis and groin may be removed.
- Cystourethrectomy: Surgery to remove the bladder and the urethra.
- Cystoprostatectomy: Surgery to remove the bladder and the prostate.
- Anterior exenteration: Surgery to remove the urethra, the bladder, and the vagina. Plastic surgery may be done to rebuild the vagina.
- Partial penectomy: Surgery to remove the part of the penis surrounding the urethra where cancer has spread. Plastic surgery may be done to rebuild the penis.
- Radical penectomy: Surgery to remove the entire penis. Plastic surgery may be done to rebuild the penis.
If the urethra is removed, the surgeon will make a new way for the urine to pass from the body. This is called urinary diversion. If the bladder is removed, the surgeon will make a new way for urine to be stored and passed from the body. The surgeon may use part of the small intestine to make a tube that passes urine through an opening (stoma). This is called an ostomy or urostomy. If a patient has an ostomy, a disposable bag to collect urine is worn under clothing. The surgeon may also use part of the small intestine to make a new storage pouch (continent reservoir) inside the body where the urine can collect. A tube (catheter) is then used to drain the urine through a stoma.
After the doctor removes all the cancer that can be seen at the time of the surgery, some patients may be given chemotherapy or radiation therapy after surgery to kill any cancer cells that are left. Treatment given after the surgery, to lower the risk that the cancer will come back, is called adjuvant therapy.
Radiation therapy
Radiation therapy is a cancer treatment that uses high-energy x-rays or other types of radiation to kill cancer cells or keep them from growing. There are two types of radiation therapy:
- External radiation therapy uses a machine outside the body to send radiation toward the area of the body with cancer.
- Internal radiation therapy uses a radioactive substance sealed in needles, seeds, wires, or catheters that are placed directly into or near the cancer. Internal radiation therapy is also called brachytherapy.
The way the radiation therapy is given depends on the type of cancer and where the cancer formed in the urethra. External and internal radiation therapy are used to treat urethral cancer.
Chemotherapy
Chemotherapy is a cancer treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping the cells from dividing. When chemotherapy is taken by mouth or injected into a vein or muscle, the drugs enter the bloodstream and can reach cancer cells throughout the body (systemic chemotherapy). When chemotherapy is placed directly into the cerebrospinal fluid, an organ, or a body cavity such as the abdomen, the drugs mainly affect cancer cells in those areas (regional chemotherapy). The way the chemotherapy is given depends on the type of cancer and where the cancer formed in the urethra.
Active surveillance
Active surveillance is following a patient's condition without giving any treatment unless there are changes in test results. It is used to find early signs that the condition is getting worse. In active surveillance, patients are given certain exams and tests, including biopsies, on a regular schedule.
New types of treatment are being tested in clinical trials.
Information about clinical trials is available from the NCI website.
Treatment for urethral cancer may cause side effects.
For information about side effects caused by treatment for cancer, visit our Side Effects page.
Patients may want to think about taking part in a clinical trial.
For some patients, taking part in a clinical trial may be the best treatment choice. Clinical trials are part of the cancer research process. Clinical trials are done to find out if new cancer treatments are safe and effective or better than the standard treatment.
Many of today's standard treatments for cancer are based on earlier clinical trials. Patients who take part in a clinical trial may receive the standard treatment or be among the first to receive a new treatment.
Patients who take part in clinical trials also help improve the way cancer will be treated in the future. Even when clinical trials do not lead to effective new treatments, they often answer important questions and help move research forward.
Patients can enter clinical trials before, during, or after starting their cancer treatment.
Some clinical trials only include patients who have not yet received treatment. Other trials test treatments for patients whose cancer has not gotten better. There are also clinical trials that test new ways to stop cancer from recurring (coming back) or reduce the side effects of cancer treatment.
Clinical trials are taking place in many parts of the country. Information about clinical trials supported by NCI can be found on NCI's clinical trials search webpage. Clinical trials supported by other organizations can be found on the ClinicalTrials.gov website.
Follow-up tests may be needed.
As you go through treatment, you will have follow-up tests or check-ups. Some tests that were done to diagnose or stage the cancer may be repeated to see how well the treatment is working. Decisions about whether to continue, change, or stop treatment may be based on the results of these tests.
Some of the tests will continue to be done from time to time after treatment has ended. The results of these tests can show if your condition has changed or if the cancer has recurred (come back).
Treatment of Distal Urethral Cancer
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of abnormal cells in the mucosa (inside lining of the urethra that have not become cancer, may include surgery to remove the tumor (open excision or transurethral resection), electroresection with fulguration, or laser surgery.
Treatment of distal urethral cancer is different for men and women.
For women, treatment may include the following:
- Surgery to remove the tumor (transurethral resection), electroresection and fulguration, or laser surgery for tumors that have not spread deeply into tissue.
- Brachytherapy (internal radiation therapy) and/or external radiation therapy for tumors that have not spread deeply into tissue.
- Surgery to remove the tumor (anterior exenteration) for tumors that have spread deeply into tissue. Sometimes nearby lymph nodes are also removed (lymph node dissection). Radiation therapy may be given before surgery.
For men, treatment may include the following:
- Surgery to remove the tumor (transurethral resection), electroresection and fulguration, or laser surgery for tumors that have not spread deeply into tissue.
- Surgery to remove part of the penis (partial penectomy) for tumors that are near the tip of the penis. Sometimes nearby lymph nodes are also removed (lymph node dissection).
- Surgery to remove part of the urethra for tumors that are in the distal urethra but not at the tip of the penis and have not spread deeply into tissue. Sometimes nearby lymph nodes are also removed (lymph node dissection).
- Surgery to remove the penis (radical penectomy) for tumors that have spread deeply into tissue. Sometimes nearby lymph nodes are also removed (lymph node dissection).
- Radiation therapy with or without chemotherapy.
- Chemotherapy given together with radiation therapy.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Proximal Urethral Cancer
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of proximal urethral cancer or urethral cancer that affects the entire urethra is different for men and women.
For women, treatment may include the following:
- Radiation therapy and/or surgery (open excision, transurethral resection) for tumors that are ¾ of an inch or smaller.
- Radiation therapy followed by surgery (anterior exenteration with lymph node dissection and urinary diversion).
For men, treatment may include the following:
- Radiation therapy or radiation therapy and chemotherapy, followed by surgery (cystoprostatectomy, penectomy, lymph node dissection, and urinary diversion).
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Urethral Cancer that Forms with Invasive Bladder Cancer
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of urethral cancer that forms at the same time as invasive bladder cancer may include the following:
- Surgery (cystourethrectomy in women, or urethrectomy and cystoprostatectomy in men).
If the urethra is not removed during surgery to remove the bladder, treatment may include the following:
- Active surveillance. Samples of cells are taken from inside the urethra and checked under a microscope for signs of cancer.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Metastatic or Recurrent Urethral Cancer
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of urethral cancer that has metastasized (spread to other parts of the body) is usually chemotherapy.
Treatment of recurrent urethral cancer may include one or more of the following:
- Surgery to remove the tumor. Sometimes nearby lymph nodes are also removed (lymph node dissection).
- Radiation therapy.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
To Learn More About Urethral Cancer
For more information from the National Cancer Institute about urethral cancer, see the following:
For general cancer information and other resources from the National Cancer Institute, visit:
About This PDQ Summary
About PDQ
Physician Data Query (PDQ) is the National Cancer Institute's (NCI's) comprehensive cancer information database. The PDQ database contains summaries of the latest published information on cancer prevention, detection, genetics, treatment, supportive care, and complementary and alternative medicine. Most summaries come in two versions. The health professional versions have detailed information written in technical language. The patient versions are written in easy-to-understand, nontechnical language. Both versions have cancer information that is accurate and up to date and most versions are also available in Spanish.
PDQ is a service of the NCI. The NCI is part of the National Institutes of Health (NIH). NIH is the federal government's center of biomedical research. The PDQ summaries are based on an independent review of the medical literature. They are not policy statements of the NCI or the NIH.
Purpose of This Summary
This PDQ cancer information summary has current information about the treatment of urethral cancer. It is meant to inform and help patients, families, and caregivers. It does not give formal guidelines or recommendations for making decisions about health care.
Reviewers and Updates
Editorial Boards write the PDQ cancer information summaries and keep them up to date. These Boards are made up of experts in cancer treatment and other specialties related to cancer. The summaries are reviewed regularly and changes are made when there is new information. The date on each summary ("Updated") is the date of the most recent change.
The information in this patient summary was taken from the health professional version, which is reviewed regularly and updated as needed, by the PDQ Adult Treatment Editorial Board.
Clinical Trial Information
A clinical trial is a study to answer a scientific question, such as whether one treatment is better than another. Trials are based on past studies and what has been learned in the laboratory. Each trial answers certain scientific questions in order to find new and better ways to help cancer patients. During treatment clinical trials, information is collected about the effects of a new treatment and how well it works. If a clinical trial shows that a new treatment is better than one currently being used, the new treatment may become "standard." Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Clinical trials can be found online at NCI's website. For more information, call the Cancer Information Service (CIS), NCI's contact center, at 1-800-4-CANCER (1-800-422-6237).
Permission to Use This Summary
PDQ is a registered trademark. The content of PDQ documents can be used freely as text. It cannot be identified as an NCI PDQ cancer information summary unless the whole summary is shown and it is updated regularly. However, a user would be allowed to write a sentence such as "NCI's PDQ cancer information summary about breast cancer prevention states the risks in the following way: [include excerpt from the summary]."
The best way to cite this PDQ summary is:
PDQ® Adult Treatment Editorial Board. PDQ Urethral Cancer Treatment. Bethesda, MD: National Cancer Institute. Updated <MM/DD/YYYY>. Available at: https://www.cancer.gov/types/urethral/patient/urethral-treatment-pdq. Accessed <MM/DD/YYYY>. [PMID: 26389384]
Images in this summary are used with permission of the author(s), artist, and/or publisher for use in the PDQ summaries only. If you want to use an image from a PDQ summary and you are not using the whole summary, you must get permission from the owner. It cannot be given by the National Cancer Institute. Information about using the images in this summary, along with many other images related to cancer can be found in Visuals Online. Visuals Online is a collection of more than 3,000 scientific images.
Disclaimer
The information in these summaries should not be used to make decisions about insurance reimbursement. More information on insurance coverage is available on Cancer.gov on the Managing Cancer Care page.
Contact Us
More information about contacting us or receiving help with the Cancer.gov website can be found on our Contact Us for Help page. Questions can also be submitted to Cancer.gov through the website's E-mail Us.
Last Revised: 2022-10-07
If you want to know more about cancer and how it is treated, or if you wish to know about clinical trials for your type of cancer, you can call the NCI's Cancer Information Service at 1-800-422-6237, toll free. A trained information specialist can talk with you and answer your questions.

